Miss a day, miss a lot. Subscribe to The Defender's Top News of the Day. It's free.
A new study by U.K. researchers sheds light on the complex nature of so-called “long COVID” symptoms in young persons. The prospective study revealed that although a percentage of people who contract COVID-19 develop persistent symptoms — and those symptoms are real — in most young people, the symptoms resolve on their own.
According to the researchers, the attribution of persistent symptoms solely to COVID-19 is ill-founded and has been exaggerated through the use of cross-sectional studies that don’t follow participants over time.
The researchers’ findings, published earlier this month in The Lancet Regional Heath — Europe, stand in contrast to the widely held perception that debilitating symptoms following COVID-19 are frequent and enduring.
Dr. Vinay Prasad, a hematologist-oncologist and professor in the Department of Epidemiology and Biostatistics at the University of California, San Francisco, offers a summary of the paper here.
Study limitations
The study involved two large groups of children and young people (CYP), ages 11-17, who were followed for a year after presenting for a COVID-19 PCR test.
Although approximately two-thirds of the participants were vaccinated, the study did not compare the incidence of long COVID symptoms with regard to vaccination status. We are thus unable to determine whether COVID-19 vaccines contribute to — or mitigate — the risk of long COVID.
Study strengths
This unique study had three important strengths. First, the incidence of symptoms among those who contracted COVID-19 is comparable to what has been shown in other studies of adolescents. This lends credibility to the results.
Second, participants in the study were observed for a full year in what is called a longitudinal study. This is in contrast to surveying people at various elapsed times since infection (a cross-sectional study).
This allows us to determine whether those who report post-infection symptoms remain debilitated or whether they get better over time.
Third, the researchers also followed a matched group of CYP who did not contract COVID-19 during the same observation period. This allowed them to estimate how many of the reported symptoms were not actually due to COVID-19 but originated from other factors present in both groups.
Findings
The study involved a sample of 5,086 non-hospitalized CYP ages 11-17. Of those, 2,909 were SARS-CoV-2-positive at baseline and 2,177 were SARS-CoV-2-negative.
The two groups matched by age, sex and geography.
Each participant in the study self-reported various symptoms of “long COVID” at zero, six and 12 months from enrollment.
The researchers assessed 21 separate symptoms. Of those, only two increased in prevalence over the 12-month observational period: shortness of breath and fatigue.
Let’s first examine these two symptoms more closely to demonstrate how this study offers something revelatory.
If, as in other studies, the prevalence of these two symptoms were simply given as a cross-section at each time, we would conclude that those unfortunate to suffer these long-haul symptoms didn’t get better and, in fact, got worse.
However, because the study was longitudinal and had a non-COVID-19 cohort, we instead see this:
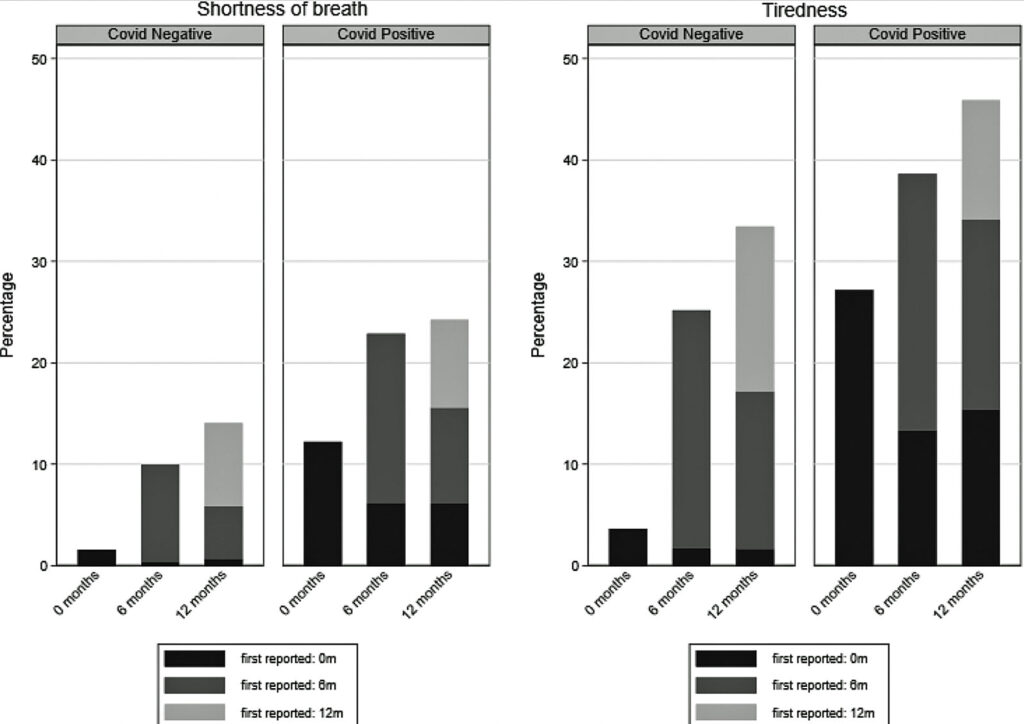
For each symptom, the percentage of those who were COVID-19-negative appears to the left of those who were COVID-19-positive. This is what we find:
- The incidence of these two symptoms in the COVID-19-positive group is higher than in the group that tested negative for the virus. This points to the fact that SARS-CoV-2 infection increases the likelihood of these two symptoms.
- The percentage of each cohort that suffers either of these two symptoms grows over the year, however …
- These symptoms increase whether or not the participant had COVID-19, and …
- Each bar in each graph is composed of three different populations — those who first reported the symptom immediately (black), those who reported the symptom only after six months (dark gray) and those who reported the symptom only after 12 months (light gray). We see that those who immediately reported the symptom got better over time.
From this, we can conclude that because the black portion of the bars in the COVID-19 group is smaller as time passes, these symptoms are resolving over time.
However, as noted above, the percentage of CYP suffering these symptoms as a whole gets larger. This is because previously asymptomatic participants are reporting new-onset symptoms six and 12 months later.
Are these new symptoms from the bout with COVID-19 experienced six and 12 months prior? This is where having a COVID-19-negative cohort becomes useful.
Because the size of the dark gray and light gray portions of each bar is roughly the same between the two cohorts, we can reasonably conclude that these delayed-onset symptoms are largely due to factors unrelated to infection.
Examining the data more closely, for symptoms initially reported, those with COVID-19 had a greater prevalence after 12 months (5.4% for shortness of breath and 13.8% for tiredness) compared to those who were COVID-19-negative.
On the other hand, the COVID-19-negative cohort reported more tiredness after 12 months than the COVID-19-positive cohort.
This pattern held true for the other measured symptoms as well. The authors state in their discussion:
“The results show that aggregating across all three time points, adverse symptoms were generally more common in test-positive compared to test-negative CYP. The majority of test-positive CYP who had a particular adverse symptom at testing were free from that symptom at both 6- and 12-months post-test, demonstrating that these symptoms generally improved over time.
“Additionally, most CYP who first developed a particular symptom 6-months after their positive (or negative) PCR-test did not report that symptom at 12-months. We also found in the sub-sample with data collected at 3-, 6- and 12-months post-test, broadly similar patterns and results.”
Long-term effects
The researchers also examined the prevalence of symptoms that manifested six and 12 months after enrollment. These cover areas of mental health, well-being and fatigue. Note the consistency between the two groups in every measure:
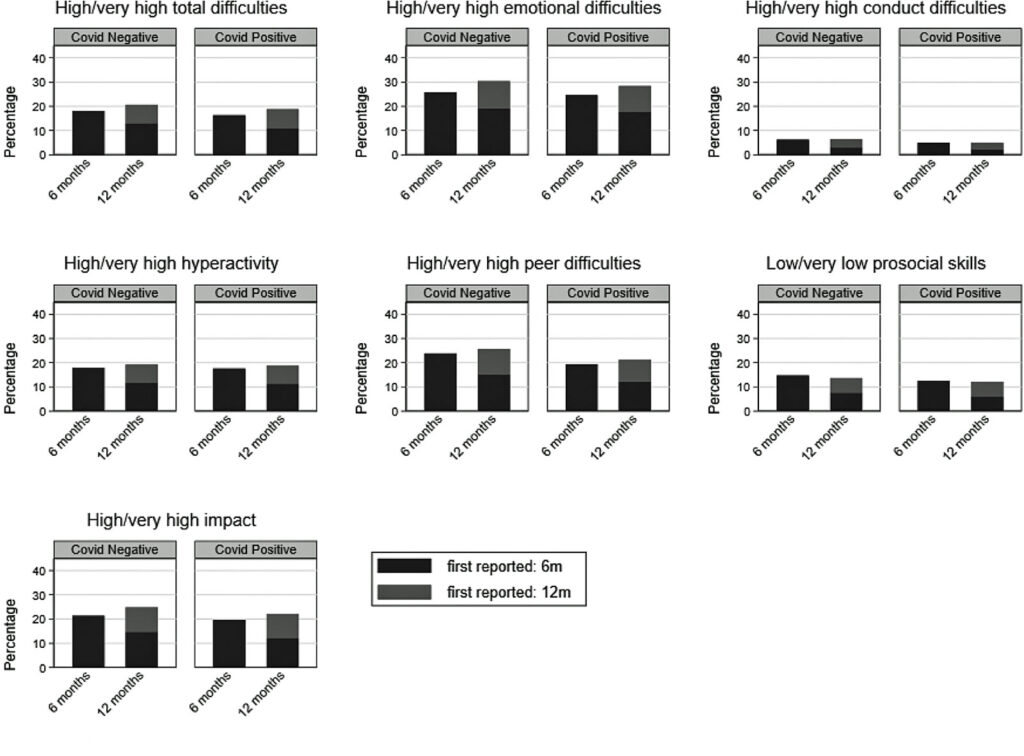
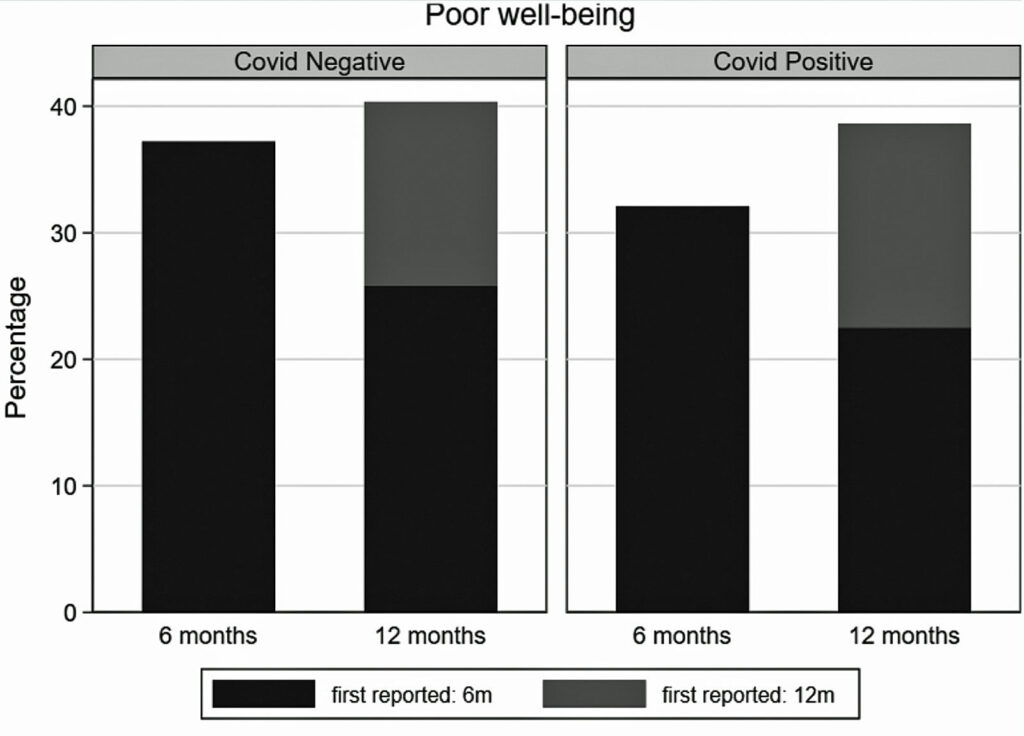
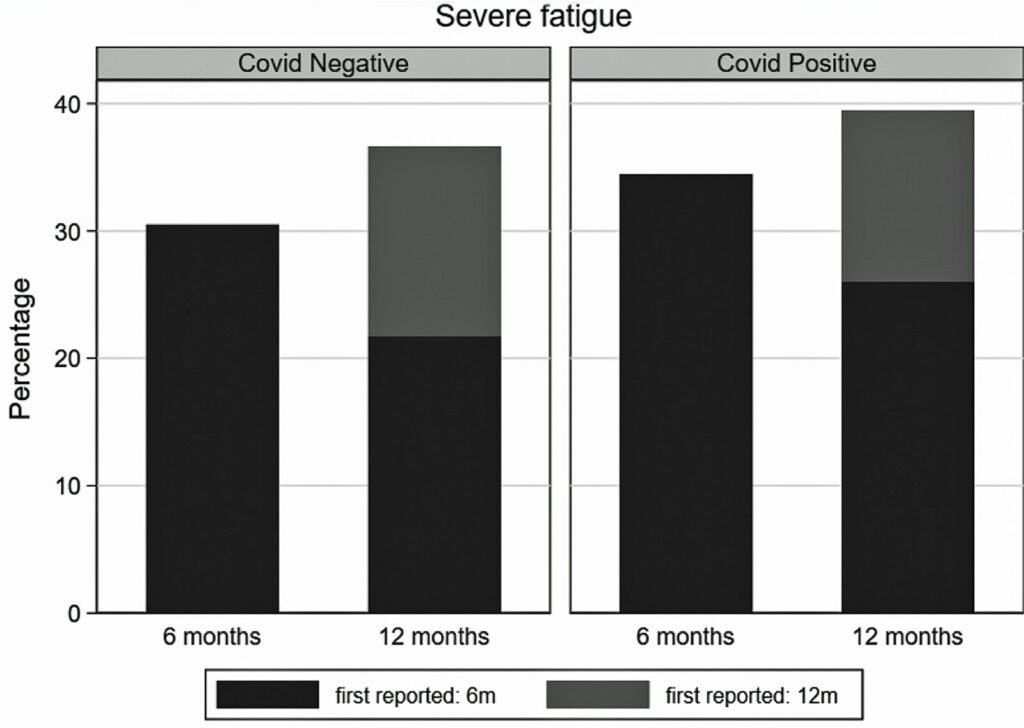
Conclusions
The authors summarize:
“Our consistent and robust findings across a diverse range of health and well-being measures emphasises (i) the close relationship between physical and mental health and (ii) the value of repeated measures over time in the same individuals.
“Taking all the data in consideration, we found that if we had simply looked at cross-sectional prevalence’s (sic) at baseline, 3- (in the sub-sample), 6- and 12-months, it would have appeared as if the prevalence of several adverse post-COVID-symptoms remained largely stable, or even increased, over time. In fact, most (but not all) CYP recovered from the adverse symptoms which they experienced at baseline and 6-months post-infection.
“However, the reporting of new onset of these same symptoms at 6- and 12-months follow-up by both test-positive and test-negative CYP suggests that these symptoms may be causally related to multiple factors and not just the original SARS-COV-2 infection. For example, the development of new symptoms 6- or 12-months after their SARS-COV-2 PCR-test in both test-positives and test-negatives could represent background levels of symptomatology in CYP in England.”





