Science Confirms (Again): Pervasive Developmental Disorder Mirrors Mercury Poisoning
When they are at their best, scientific journals can offer a receptive forum for the exchange of ideas, and an opportunity to put forth or debate specific hypotheses in an open-minded manner. Within this forum, some scientific claims may vie for the status of “canonized facts”—and some may even come close to achieving that status—but always, there should remain the possibility of re-examining a claim’s veracity.
Unfortunately, the careful weighing of scientific evidence can be led astray by conflicts of interest and agency agendas. Since the early 2000s, the Centers for Disease Control and Prevention (CDC) and other federal agencies have assiduously tried to enshrine and “canonize” as unassailable “fact” their dubious claim that mercury (and particularly the vaccine preservative thimerosal) have nothing to do with autism or other pervasive developmental disorders (PDDs). For decades, this position has required the agencies to ignore a sizeable body of evidence to the contrary—including the Institute of Medicine’s (IOM’s) determination in 2001 that an autism-mercury association is “biologically plausible”—while discrediting authors who persist in making the mercury-PDD case. Thus, after a Medical Hypotheses commentary described compelling and extensive parallels between mercury poisoning and autism in the same year as the IOM report, the industry-beholden journal Pediatrics solicited an aggressive rebuttal (Nelson & Bauman 2003) that dismissed the parallels as “improbable.” Despite the continuing accrual of evidence outlining mercury’s probable causal or contributory role in PDD brain pathology, the 2003 rebuttal set the tone for the government’s persistent denials of harm.
Reconsidering biological plausibility
One of the key features of the Nelson/Bauman rebuttal was the authors’ assertion that the medical conditions associated with mercury exposure are wholly distinct from the medical conditions associated with PDDs. Now, 15 years later, a study in Metabolic Brain Disease essentially demolishes that argument, instead reconfirming “the biological plausibility of mercury poisoning to induce PDD diagnoses.”
Using nationally representative health maintenance organization (HMO) data from 1991–2000 (a decade when thimerosal-containing vaccines were in heavy use), the new study compares two groups of children: (1) children diagnosed with at least one PDD, and (2) children without a PDD diagnosis. To ascertain the potential overlap between symptoms of mercury poisoning and PDD, the researchers then look at the initial occurrence—before the PDD diagnosis—of five medical conditions acknowledged by Nelson and Bauman to be associated with mercury poisoning.
The results are unequivocal: compared to children without a PDD, children with a PDD “have a significantly greater frequency of receiving a medical diagnosis associated with [mercury] poisoning…preceding their eventual PDD diagnosis”:
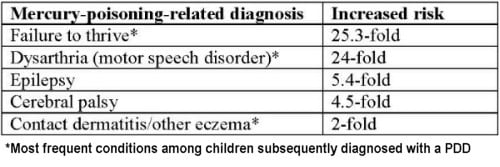
The researchers also discuss other recently published studies that not only confirm their findings for the five conditions above but show comparable magnitude and direction of results for a handful of other conditions admitted by Nelson and Bauman to be signs of mercury poisoning (including ataxia, constricted visual fields, fetal malformations, peripheral neuropathy and psychiatric symptoms). Considering these multiple strands of evidence, what is the researchers’ overall conclusion?
“Direct evidence from this study and recent studies published in the scientific literature support a [significant] link in twelve of twelve categories (100%) of [mercury] poisoning-associated symptoms as defined by Nelson and Bauman…and symptoms observed in those with a PDD diagnosis” [emphasis added].
Hard-to-deny results
When some of the original Medical Hypotheses authors had the opportunity to publish a critique of the Nelson/Bauman paper back in 2004 (although not in Pediatrics, which denied them the right of response), the critique pointed out that Nelson and Bauman were disingenuous to limit the “typical and characteristic manifestations” of mercury poisoning to a small list. In fact, “expert toxicologists well know [that] ‘no other metal better illustrates the diversity of effects caused by different chemical species than does mercury.’” Toxicologists also know that myriad factors play into mercury toxicity, including amount of exposure, dosing patterns, mercury species type, route of administration, excretion capacity, age and developmental context.
While acknowledging these complexities, the 2018 study makes a powerful case precisely because it restricts its focus to the specific symptoms of mercury poisoning cited by the Pediatrics authors, showing that each and every one overlaps significantly with PDDs. Although CDC and the medical-pharmaceutical industry may continue to plant the claim of “no mercury-PDD relationship” within the compliant mainstream media, more scrupulous scientists and clinicians will not be able to ignore this latest evidence of mercury’s role in PDD pathogenesis.
Sign up for free news and updates from Children’s Health Defense. CHD focuses on legal strategies to defend the health of our children and obtain justice for those injured. We can't do it without your support.


