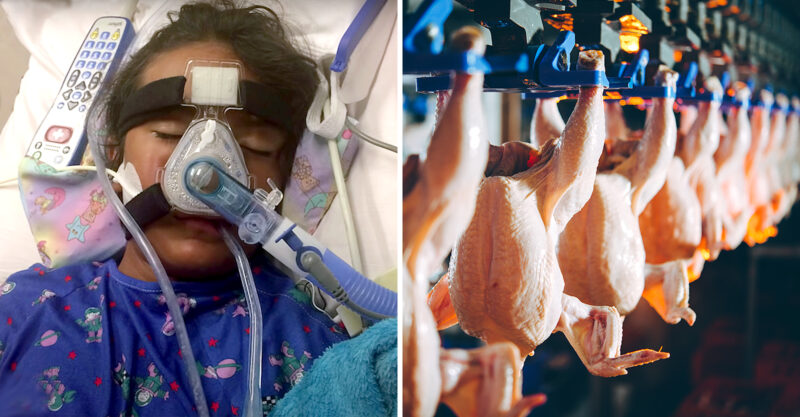
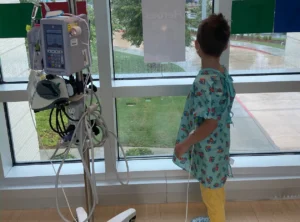
Joanne Canda-Alvarez found her 9-year-old son splayed out on his bedroom floor, unable to move and foaming at the mouth. The day before, Jayven had been playing golf with his family.
Now he was completely paralyzed by the sudden onset of a rare autoimmune disease that doctors linked to campylobacter, a bacteria mainly found in poultry products.
Canda-Alvarez and her husband did not know whether their son would survive — he was on a ventilator in hospital and unable to even speak. But his mother could see how scared he was. “I could tell it in his eyes,” she said.
Nearly four years after falling sick, Jayven still struggles to control his hands and his right foot, a result of lasting nerve damage. “Nobody has an answer to if he’ll ever recover fully — if his body will ever be the same,” said his mother.
Campylobacter is America’s biggest cause of foodborne illness, just ahead of salmonella. Both are potentially fatal.
Yet between 2015 and 2020, U.S. companies — including the poultry giants Perdue, Pilgrim’s Pride, Tyson, Foster Farms and Koch Foods — sold tens of thousands of meat products contaminated with campylobacter and salmonella, according to government sampling records obtained by the Bureau of Investigative Journalism.
More than half of these were contaminated with antibiotic-resistant strains — a rapidly escalating issue that can be exacerbated by poor hygiene conditions.
The poultry companies supply major grocery stores and fast-food chains. Tyson has supplied chicken to McDonald’s, Perdue has sold to Whole Foods and both have supplied Walmart.

Although the U.S. Department of Agriculture (USDA) deems a certain level of salmonella and campylobacter within poultry acceptable, 12 major U.S. poultry companies, including Perdue, Pilgrim’s Pride, Koch Foods, Foster Farms and Tyson, have exceeded USDA standards for acceptable levels of salmonella multiple times since 2018, when the government began reporting contamination rates at individual plants, according to the department’s records.
The USDA still runs tests for campylobacter in processing plants but it is not currently tracking whether plants exceed the contamination thresholds.
Batches of poultry products with contamination rates above the limit don’t have to be recalled, although plants that repeatedly exceed the thresholds can be temporarily shut down.
Separate government records also show that between January 2015 and August 2019, the same 12 major U.S. poultry companies broke food safety rules on at least 145,000 occasions — or on average more than 80 times a day.
Poultry plant workers also claimed they have sometimes been asked to process rotten-smelling meat, have witnessed chicken tossed into grinders with dead insects and found government safety inspectors apparently asleep on the job.
“Since [the meat] comes to us really dirty, when we open the box, it’s like, ‘Let’s see what’s inside!’” alleged one worker at a Tyson plant in Springdale, Arkansas.
“Sometimes it has flies, it has crickets, cockroaches in there already frozen.” He claimed that when he pointed this out to the supervisors, they seemed to show little interest — and so the insects ended up being put into the grinder with the meat.
Campylobacter causes more than 100 deaths every year in America as well as 1.5 million infections. It also accounts for up to 40% of the country’s cases of Guillain-Barré Syndrome, the disease that left Jayven paralyzed.
Yet the sale of poultry products found to be contaminated with either that or salmonella bacteria remains perfectly legal.
Canda-Alvarez is still shaken by her son’s experience. “One day he’s playing golf, and the next day he’s completely paralyzed. It was the most mind-boggling thing I’ve ever experienced,” she said.
“When they told me that it was from campylobacter I was like, ‘So this bacteria that nobody knows about, that could destroy your whole life, is from chicken or poultry?’
“That’s why I tell people, you need to be careful how you cook your food or where you eat. Because you never know what could happen.”
The level of salmonella and campylobacter that the USDA deems acceptable differs depending on the product. A maximum of 15.4% of chicken parts leaving a processing plant, for instance, can test positive for salmonella and the plant can still meet acceptable standards.
The threshold for campylobacter is 7.7%. Many experts argue these levels are too lax.
The USDA’s Food Safety and Inspection Service (FSIS) does “a very poor job of regulating the contaminants,” according to Zach Corrigan, senior staff attorney at the pressure group Food & Water Watch.
“This comes in the way of allowing super-fast line speeds, allowing companies to largely regulate themselves on the slaughter and then doing very little monitoring of contamination.”
An FSIS spokesperson said: “FSIS is committed to reducing foodborn infections associated with FSIS-regulated products, including reduction of salmonella illnesses attributable to poultry.”
Especially concerning is the increase in antibiotic-resistant strains of bacteria. The number of drug-resistant salmonella infections in the U.S. rose from around 159,000 in 2004 to around 222,000 in 2016, according to the CDC.
Campylobacter has become more resistant too: ciprofloxacin, an antibiotic commonly used to treat it, is increasingly ineffective.
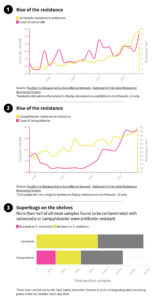
The bureau has uncovered a catalog of hygiene breaches, many of them at plants run by large U.S. poultry firms linked to the supply of superbug-infected meat — and these conditions have “a huge impact” on drug-resistant bacteria, said Mohammad Aminul Islam, assistant professor at Washington State University’s School for Global Health.
“In a slaughterhouse, you have lots of poultry coming from different places,” he said. “So you don’t know which is from a good farm, which is a less clean farm, which is more colonized [by drug-resistant bacteria], which is less colonized. But they are just mixed together. So the processing plant hygiene and environmental condition is a critical point.”
The rise of superbugs is having increasingly serious human consequences. Antibiotics have been used effectively against these bacterial diseases but due to drug resistance, doctors are turning more frequently to last-resort drugs, which often have more side effects.
And if these fail, there is no choice but to let the disease take its course.
‘You don’t think a drive-through could cost your kid their life’
Ashley Queipo believes an impromptu trip to Chick-Fil-A in April 2020 likely resulted in her son fighting for his life. After a long morning of home-schooling in their town of Brooksville, Florida, the family headed to the drive-through as a treat.
Eight-year-old Chace ordered his favorite: chicken nuggets. But within hours, he fell seriously ill. When he was hospitalized with salmonella, tests showed the infection was resistant to all antibiotics.
“You don’t think that going through a drive-through and handing that brown paper bag to your kid in the back seat could cost them potentially their life,” said Queipo. “But that is the reality.” She believes the nuggets made him sick. It was one of the last meals he ate before falling ill and the only one neither of his parents prepared.
Queipo did not report the incident to the restaurant because the family initially thought the illness was caused by a virus and by the time it was diagnosed as salmonella, she was focused on her son’s condition. Chick-Fil-A declined to comment.
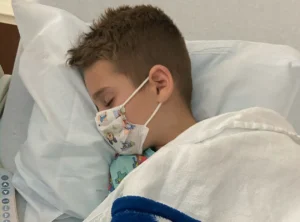
“The odds were really against him,” Queipo remembered. “He was so dehydrated, he had a fever and he was hallucinating. His body was trying so hard to fight it. And it just couldn’t.”
Chace’s stomach and bowels stopped working, but doctors were left with no treatment options beyond inserting a tube into a vein near his heart to give him nutrition.
Chace was lucky: he recovered to full health — albeit over four months. These days he no longer eats nuggets and is anxious about eating meat at all. “We don’t eat out anymore,” said his mother. “We very rarely eat chicken. If we do, we overcook it.”
The recent rise of campylobacter and salmonella in chicken can be traced back to the birth of industrial poultry farming.
Today chicken is America’s favorite meat, but before the second world war, it was expensive and eaten largely by the wealthy. The average American ate no more than 10 pounds a year — about a tenth of what is consumed today.
Wartime rationing of beef, lamb and pork changed this temporarily. But when that came to an end, Americans were ready to once again abandon costly poultry products.
Fearing this eventuality, one savvy supermarket chain, supported by the USDA, launched a contest to breed “the chicken of tomorrow.”
The plan worked — by the 1950s, the contest had produced a fatter, faster-growing hybrid breed of bird — and kickstarted the industrial chicken-farming system that exists today.
Antibiotics catalyzed this chicken boom. The drugs had transformed human healthcare after they became widely available in the 1940s, but farmers soon discovered that antibiotics do not only curb disease, they also stimulate growth in animals.
It was not long before America’s poultry producers were pumping antibiotics into animals at all stages of production, be it injections given to day-old chickens or drugs put in feed to fatten up broiler birds.
Antibiotics also helped suppress the diseases common in industrially farmed birds that were reared in cramped and unsanitary conditions.

University Archives Photograph Collection, Agricultural Extension and Research Services Photographs, UA023.007, Special Collections Research Center, NC State University Libraries, Raleigh, NC
Certain procedures changed over time and some rules have been tightened in recent years — U.S. Food and Drug Administration regulations now ban the use of the drugs on animals to promote growth — but the consequences of antibiotic overuse are still being felt today.
Some studies from Europe have shown that it can take at least eight years for resistant strains of bacteria to decline after antibiotic use is curtailed.
Bacteria evolve to develop resistance to the antibiotics attacking them — the more the drugs are used, the more resistance to them rises.
As such, antimicrobial resistance has become a major cause of death, directly killing an estimated 1.27 million people in 2019 and linked to almost 5 million deaths around the world, according to a recent study published in the Lancet.
In America, antibiotic-resistant superbugs kill more than 35,000 people each year and make another 2.8 million sick.
As fears about drug resistance have mounted, U.S. poultry firms have cut their use of antibiotics. “The chicken industry for years has been a leader in reducing usage,” a spokesperson for the National Chicken Council told the bureau.
Yet experts say stricter measures are still required to contain drug-resistant bacteria, especially around hygiene. Under the current system, animals are slaughtered at “amazingly fast speeds with little regard for sanitation,” said Corrigan.
“And the pathogens that are in these animals’ bodies get spread everywhere, and these pathogens are increasingly resistant to antibiotics. And then we’re all exposed.”
Anything but wholesome
At a Tyson plant in Springdale that deals with turning chicken meat into nuggets and burgers, boxes of chicken have sometimes arrived “rotten,” alleged one worker.
He added: “We notified the supervisor. We said, ‘Hey this chicken stinks, it smells awful.’ He says, ‘No, toss it in.’”
The plant “smells like a rotting animal,” the worker claimed — meat has been left stuck in machines, which were not properly washed because the company responsible for cleaning is short-staffed.
“There’s meat everywhere, laying on the floor,” he alleged. But rather than being thrown away he claimed it was washed and added back into the processing line.
Sitting on a foldout chair in his sparsely furnished living room, the worker described his concerns of potential consequences for speaking publicly. He was worried management might try to find an excuse to fire him if he was found out, he said in a hushed voice, just audible over the noise of kids’ cartoons coming from the next room.
Another worker from the plant claimed that he had seen the Food Safety and Inspection Service officials, who are in the plant to guarantee hygiene standards, sleeping on the job.
Tyson Foods denies acting inappropriately. “Tyson Foods has been serving American families safe, nutritious food for nearly a century, and we categorically reject the allegations leveled,” said a company spokesperson, adding that the plants in question have received the highest ratings from a third-party auditor that oversees food safety standards.
“Our team members have a number of ways to raise concerns without fear of retaliation. Beyond raising concerns to their supervisors, management, and human resources they can also anonymously report issues to our helpline.”
Despite unhygienic conditions at plants, companies have been able to market their food as clean and virtuous using “outright deceitful” images, claimed Corrigan at Food & Water Watch.
“[Companies] know that consumers want to not only have a product that is safe for themselves and their families, they also want a product that is sustainably and justly raised. And the industry plays on that with pictures of idealized family farms, where every chicken is a happy chicken,” he said.
Poultry companies like to advertise their meat as “wholesome” — a label given by USDA inspections. Yet the Physicians Committee for Responsible Medicine carried out a study in 2011 that found fecal bacteria in almost half of 120 chicken products sold by 15 supermarket chains in 10 U.S. cities.
The group petitioned the USDA to drop the word “wholesome” from the inspection labels of poultry products contaminated with fecal matter but after being taken to court for its failure to respond, the USDA denied the petition.
The USDA conceded that bacteria from feces are routinely found in poultry products but argued no action needed to be taken as it only deems feces visible to the naked eye as an “adulterant” — a substance that compromises the product’s safety.
So, “wholesome” chicken, contaminated with fecal matter, continues to be sold on supermarket shelves across the U.S.
“Poultry companies have invested tens of millions of dollars annually in technology and other scientifically validated measures to enhance the safety profile of chicken products,” said a spokesperson for the National Chicken Council. He added that the vast majority of broiler chicken plants met the government performance standards.
USDA records obtained by the bureau, however, identify a number of cases in which individual slaughterhouses breached hygiene regulations hundreds of times.
One Tyson slaughterhouse in Springdale — responsible for dozens of poultry products contaminated with drug-resistant campylobacter — was found to have breached food safety and hygiene regulations more than 800 times between 2015 and 2020.
In one instance, inspectors reported that birds arrived at the plant dead but were still put into the production line, which is prohibited by sanitary regulations. In others, chickens were found to be contaminated with fecal matter.
On the same day that one report of fecal contamination was made, a batch of chicken tested positive for drug-resistant campylobacter.
The reports are documented “non-compliances,” or failures to meet the requirements of government regulations. Companies can contest the validity of these breaches, but none of the businesses contacted for this story said that they had.
A Tyson Foods spokesperson said: “Both Tyson and USDA inspectors are trained to take immediate action when a food safety concern is detected. If a product does not meet federal safety standards, it’s immediately removed from production.”
Need for reform
High rates of COVID infections among poultry workers have also put the spotlight on the conditions in processing plants.
Line-speed waivers — which allow plants to accelerate processing times beyond the federally capped 140 birds per minute — have come under particular fire from workers’ rights groups who argue faster speeds require more workers, which could impinge social distancing.
Increasing line speeds can also have knock-on effects on hygiene and disease control, said Magaly Licolli, director of Venceremos, an Arkansas-based poultry workers’ rights group.
The Tyson plant in Arkansas, which committed numerous hygiene breaches and produced chicken contaminated with drug-resistant bugs, was granted a line-speed waiver in September 2018.
More recently, she said, the USDA has sanctioned these increases while inspections have declined.
“With less inspectors and the chicken coming faster,” she said, “it’s impossible for any human being to catch the bird that comes in sick.”
Poultry companies are given the results of tests carried out on samples. But under current regulations, no strain of campylobacter or salmonella is classified as an adulterant.
This means that companies have no legal obligation to withhold batches of food contaminated with campylobacter or salmonella — even drug-resistant variants — or to recall meat already sold. These products could be knowingly and legally sold to customers for human consumption.
This is a “travesty from a public health standpoint,” said David Wallinga, senior health adviser at the Natural Resources Defense Council.
Wallinga said that the approach in America has long been to simply accept that millions of people getting food poisoning each year is “just the price we pay for having big meat industries and pretty inexpensive sources of meat.”
He said the outbreaks of food poisoning caused by antibiotic-resistant strains have been “the gorilla in the room.”
For families hit by the worst consequences of these diseases, the lax regulations are hard to accept. “It’s actually really upsetting because they are still selling [poultry products] to these people,” said Joanne Canda-Alvarez. “And they are not making people aware of what could happen.”
“Everybody knows about salmonella,” she added. ”We didn’t learn about [campylobacter] even until he got it. It’s a dangerous bacteria. It’s a bacteria that can do very bad things to you.”

Campaigners and politicians have stepped up the pressure for legal reform to classify certain strains of salmonella as adulterants, which would force companies to withdraw products that test positive from sale.
Bill Marler, a food safety attorney, recently threatened to “proceed with judicial remedies” against the USDA if officials fail to respond to his petition made last January for 31 strains of salmonella to be made adulterants.
In September 2021, the Center for Science in the Public Interest sent another petition to the USDA, calling for enforceable standards that target the bacteria posing the greatest risk to human health. Several big firms, including Tyson and Perdue, signed the letter.
“Food safety, farmer relationships and animal care are top priorities for us at Perdue,” said a spokesperson for the company. “That’s why our company advocates for the modernization of our nation’s food safety regulations and welcomed recent steps by USDA to address these concerns in a way that utilizes the most up-to-date science.”
Koch Foods, Foster Farms, Pilgrim’s Pride, McDonald’s and Walmart did not respond to requests for comment. Whole Foods declined to comment.
A 2010 study into campylobacter found that poor health and welfare among chickens also impairs their ability to control infections. Stress hormones trigger the rapid growth of campylobacter bacteria and enable it to move out of the gut and into the bird’s muscle tissue — the parts that humans eat.
There is no formal regulation of farm conditions in the U.S., and therefore no government inspection records, but whistleblowers and undercover investigators have reported that farms have often been filthy and hugely overcrowded, with tens of thousands of birds packed into windowless sheds.
A complaint filed with the Bureau of Consumer Protection from February 2021 documented the traumatic catching process, detailing how Tyson sends “catching crews” into the grow houses to grab the chickens that are big enough for slaughter.
The catchers “grab the birds by the legs and carry them upside down by their ankles — multiple birds in each hand — before pushing them into the transport cages,” the complaint said. The cages are not tall enough for the birds to stand upright and so many birds are packed into each that they do not have room to move or spread their wings.

Rudy Howell, who reared chickens for Perdue from 1994 until summer 2020, has also made a series of allegations about the company. In 2021 Howell filed a complaint to the Occupational Health and Safety Administration against Perdue for alleged wrongful discharge after he spoke out about their practices.
Perdue disputes his allegations and accuses him of having breached biosecurity measures by inviting a film crew onto his farm.
Howell’s allegations related to inadequate hygiene and disease control measures, including the claim that Perdue sometimes delivered chicks in dirty trays and used dirty machines to catch chickens.
A spokesperson for Perdue said: “Food safety, farmer relationships and animal care are top priorities for us at Perdue. Our 101-year-old business is built on attention to detail at every step of our supply chain, as well as trust and collaboration with the farmers who raise our animals.”
Howell told the bureau he never received any information about whether tests for diseases had been carried out before the chicks were delivered to his farm. Tests were not always carried out after he alerted the firm about the worrying rates of illness among new flocks, he added.
“You don’t get nothing. You just pick up dead birds. That’s all they do is tell you to pick up the dead birds,” Howell said.
Originally published in The Bureau of Investigative Journalism.